If your sinuses feel fine during the day but unbearable at night, there are specific reasons why — and specific fixes that actually work. Here’s the full breakdown.

You made it through the day. Sinuses weren’t great, but they were manageable. You go to bed, you lie down, and within twenty minutes your nose is completely blocked. You’re breathing through your mouth. Your face feels packed with pressure. Sleep feels impossible. You get up, blow your nose, get nothing, and go back to bed to start the cycle all over again.
If this is a nightly ritual for you, you’re not imagining it and you’re not unlucky. There are very specific, well-understood reasons why sinus congestion reliably gets worse at night — and once you understand them, the fixes become a lot more obvious than just “try to push through it.”
The Main Reason: Gravity Stops Working For You
During the day, whether you’re sitting, standing, or moving around, gravity is on your side. Your sinuses drain downward and forward. Mucus keeps moving. Pressure doesn’t build up in one place for too long.
The moment you lie flat, that drainage system stalls. Mucus that was flowing during the day now has nowhere to go — it pools in your nasal passages and sinus cavities, the tissue lining your nose swells with increased blood flow from the horizontal position, and what was mild congestion during the day becomes full blockage within minutes of lying down.
This is also why so many people find that one nostril blocks up completely while the other stays clearer — and then they switch sides during the night and the opposite nostril takes over. That’s your body’s nasal cycle doing exactly what it’s supposed to do, just more noticeable because you’re horizontal and the swelling is amplified.
The fix for this particular problem is straightforward: sleep with your head elevated. Not sitting-up elevated, but enough of an angle to keep drainage moving. An extra pillow or a wedge pillow under your head and upper back — even just a few inches of elevation — makes a meaningful difference in how your sinuses drain through the night. If you’ve been through septoplasty recovery, you already know this one well — it’s standard post-op advice for exactly this reason.
The Air in Your Bedroom Is Probably Making It Worse
This is the one most people don’t think about, and it’s often the biggest leverage point for actually changing how you sleep.
While you’re awake and moving through your day, you’re breathing a mix of indoor and outdoor air, you’re staying hydrated, and your nasal passages are staying relatively active. At night, you spend seven to nine hours breathing whatever is specifically in your bedroom — the same air, recycled, the entire night. If that air is dry, dusty, or loaded with allergens, your sinuses are taking a sustained hit for hours with no break.
Dry Air Is Silently Wrecking Your Sleep
Dry air is probably the most common and most underestimated nighttime sinus trigger. Your nasal passages need moisture to function properly. The cilia — tiny hair-like structures that sweep mucus and debris through your sinuses — work best in a specific humidity range. When the air is too dry, mucus thickens, cilia slow down, the nasal lining gets irritated and swells in response, and congestion worsens. This is especially brutal in winter when heating systems run continuously and strip moisture from indoor air for months at a stretch.
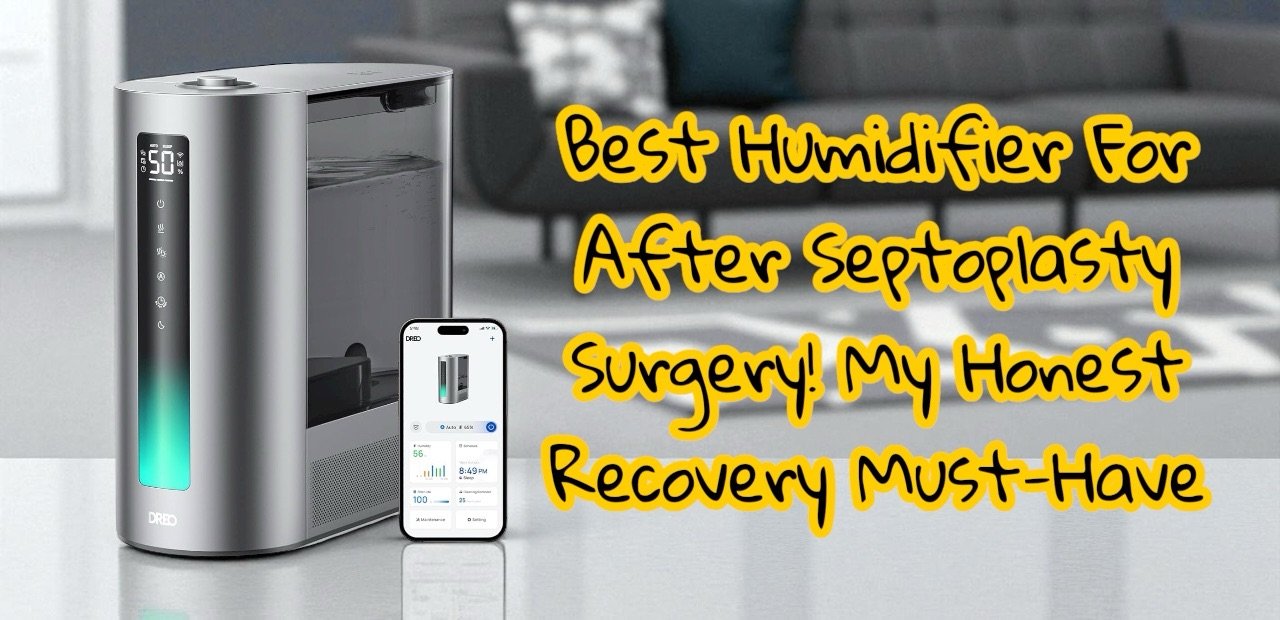
Running a humidifier in your bedroom while you sleep is one of the most impactful single changes you can make for nighttime sinus congestion, and the effect is often noticeable within the first night or two. The key is having the right one — something quiet enough not to disturb your sleep, with enough capacity to run through the night without needing a refill, and ideally with smart humidity control so it doesn’t over-humidify. A smart humidifier with auto humidity sensing handles that last part for you, which matters more than it sounds — too much humidity creates its own problems, including encouraging dust mite populations and mold growth. If you had septoplasty, a humidifier wasn’t optional during recovery, and the same logic applies here: dry air and healing nasal tissue simply do not get along.
Your Bedding Might Be the Allergen Source
Dust mites are microscopic creatures that live in mattresses, pillows, and bedding, and they are one of the most common triggers for people who experience chronic nighttime sinus congestion and wake up feeling like they’ve been hit by a truck. You don’t need to be dramatically allergic to dust mites for them to affect you — even a moderate sensitivity, combined with eight hours of direct exposure, is enough to cause significant nasal inflammation by morning.
Mattress and pillow encasements that create a physical barrier against dust mites — like the allergen-barrier covers discussed here — are a one-time change that reduces your nightly allergen exposure significantly. They’re not glamorous, but they’re one of the highest-impact passive interventions for people whose sinus congestion is worst in the morning and improves as the day goes on — that morning-worst pattern is a classic sign that your sleep environment is the trigger.
Airborne Allergens and Irritants in the Bedroom
Beyond dust mites in the bedding, the air itself in most bedrooms carries a meaningful load of particulates — pet dander if you have animals, mold spores if there’s any moisture issue in the room or the building, dust from carpets, curtains, and surfaces that gets disturbed and becomes airborne throughout the day. All of it gets breathed in while you sleep.
An air purifier with a true HEPA filter running in your bedroom is the most direct way to address this. HEPA filtration captures particles down to 0.3 microns — that includes pet dander, dust mite debris, mold spores, and pollen — and what it removes from the air doesn’t end up in your nasal passages while you’re trying to sleep. A quality HEPA air purifier in the bedroom is one of the most consistently recommended environmental changes for people with chronic sinus issues, and if you want to understand exactly what’s in your bedroom air before committing to a purifier, an indoor air quality monitor will show you particulate levels, humidity, and volatile compounds in real time. The numbers are often surprising.
Blood Flow Changes When You Lie Down
Here’s something most people don’t know: the tissue lining the inside of your nose is erectile tissue, meaning it fills with blood in response to certain signals — horizontal position being one of them. When you lie down, blood pools more easily in the vessels of your nasal lining, the tissue swells, and the already-narrow nasal passages get narrower. This is a normal physiological response, but if your nasal passages are already compromised by inflammation, a deviated septum, or swelling from allergies or a sinus condition, that normal nighttime swelling pushes you from “manageable” to “completely blocked.”
This is exactly why people who feel fine during the day — or only mildly congested — can find themselves unable to breathe through their nose at all the moment they get horizontal. It’s also part of why even mild chronic sinusitis creates such disproportionate sleep disruption. The nighttime blood flow shift amplifies whatever is already happening in your sinuses.
Post-Nasal Drip and the Cough That Won’t Let You Sleep
Nighttime congestion often comes packaged with post-nasal drip — mucus draining down the back of the throat instead of out through the nose. During the day, you swallow constantly without thinking about it and most of that drainage goes down without causing problems. Lying flat changes the angle, and that drainage pools at the back of the throat instead of moving through it. The result is the maddening nighttime cough or throat-clearing that wakes you up, wakes your partner up, and makes it nearly impossible to settle into real sleep.
Elevation helps here too, for the same gravitational reason. Keeping your upper body slightly raised encourages the drainage to move down the throat and into the stomach rather than pooling at the top. Staying well hydrated throughout the day also matters more than people realize — when you’re adequately hydrated, mucus stays thinner and drains more easily rather than thickening and sitting in the back of your throat. The connection between hydration and sinus drainage is direct and underappreciated, and the people who address it consistently notice a real difference in nighttime symptoms.
Allergies Hit Differently at Night
If allergies are part of your sinus picture — and for a lot of people with chronic nighttime congestion, they are, even when they’re not fully aware of it — nighttime creates specific conditions that make allergen exposure worse.
Pollen levels peak in the morning and again in the evening, so if you’re sleeping with windows open during spring and summer, you’re breathing peak pollen during your sleep window. Indoor allergens are another story — dust mites, mold, and pet dander don’t have a season, and your bedroom is often the highest-concentration environment for all three because it’s where you spend the most time and where ventilation is lowest.
There’s also a circadian rhythm to your immune response. Certain immune chemicals that drive allergic inflammation follow a daily cycle, with levels naturally higher in the early morning hours — which aligns with why so many allergy and asthma sufferers feel worst between 3 and 6 AM. It’s not just the environment, it’s the body’s own inflammatory rhythm.
If you suspect allergies are behind your nighttime sinus problems, the bigger picture of why chronic sinusitis keeps returning covers the allergy-sinusitis connection in detail and is worth reading alongside this one.
The Mouth Breathing Spiral
When your nose is blocked at night, you breathe through your mouth. Mouth breathing dries out your throat and airway, which causes more irritation and inflammation, which makes your sinuses respond with more mucus, which increases the congestion, which keeps you mouth breathing. It’s a feedback loop that compounds through the night and leaves you feeling worse in the morning than when you went to bed.
Breaking that loop at the source — reducing the nasal congestion so you can actually breathe through your nose — is the real goal. But in the meantime, nasal strips that gently open the nasal valve and increase airflow can make a meaningful difference. They don’t address what’s causing the congestion, but they can keep airflow through the nose open enough to reduce the mouth breathing spiral. Extra-strength nasal strips are one of those low-tech solutions that genuinely work well for a lot of people as a nighttime band-aid while the underlying issues are being addressed.
Steam Before Bed: Why It Works
A lot of people notice that their sinuses feel noticeably better immediately after a hot shower — the steam loosens thick mucus, reduces swelling in the nasal lining, and creates a brief window of real relief. Taking your shower at night rather than in the morning is a simple, zero-cost way to start your sleep window with your sinuses at their most open.
You can extend that effect with shower steamers that contain eucalyptus and peppermint — the menthol and cineole compounds in those oils have a genuine vasodilatory effect on nasal passages and can extend the steam’s relief into your first hour of sleep. Eucalyptus shower steamers are one of those things that seem too simple to matter but get genuinely enthusiastic responses from people who use them regularly for this purpose.
If you want more targeted relief than a shower can provide, a portable steam inhaler gives you the same benefit in a more concentrated form — something you can use for ten minutes right before getting into bed to open things up before you lie down. The Vicks portable steam inhaler is worth knowing about if nighttime congestion is serious enough that you’re lying there unable to sleep.
Sinus Rinsing in the Evening: The Timing Matters
If you’re already doing nasal irrigation — and if you deal with chronic sinus congestion you really should be — the timing of when you do it affects how much benefit you get overnight. Rinsing in the morning is better than not rinsing at all, but rinsing in the evening, an hour or so before bed, clears out the allergens and irritants that accumulated throughout the day before you seal yourself into your bedroom for eight hours. You go to sleep with cleaner nasal passages, lower allergen load, and better drainage to start the night.
If you’re not yet using an electric irrigator and still relying on a squeeze bottle or neti pot, the difference in thoroughness and comfort is significant — especially for evening use when you want the rinse to be effective enough to actually matter through the night. A proper electric sinus rinse machine makes evening irrigation something you’ll actually stick with rather than something you do twice and abandon because it hurts or makes a mess.
What About Decongestant Nasal Sprays at Night?
A lot of people reach for decongestant sprays like oxymetazoline when nighttime congestion gets bad enough. They work fast, they work well, and that’s precisely the problem — they work so well that people use them night after night, and after three to five days, the nasal passages become dependent on them to stay open. When you stop using the spray, the rebound congestion is often worse than the original problem. This is called rhinitis medicamentosa, and it’s incredibly common and genuinely miserable to get out of.
If you’re going to use a decongestant nasal spray, use it for two to three nights maximum during an acute flare and then stop. It’s not a nightly maintenance tool. The approaches outlined throughout this article — humidifier, air quality, allergen reduction, elevation, irrigation — are the sustainable nighttime management strategy. The spray is for emergencies, not habits.
Saline nasal sprays are a different story — no rebound, no dependency, and they genuinely help keep the nasal lining moist overnight, which reduces the dry-air swelling cycle described earlier. A few sprays of plain saline before bed is a useful addition to any nighttime sinus routine.
When Nighttime Congestion Points to Something Bigger
For most people, the nighttime worsening of sinus congestion is a manageable problem that responds well to the environmental and behavioral changes described above. But persistent, severe nighttime congestion that isn’t responding to any of these approaches can point to something that warrants medical attention.
A significantly deviated septum — where the cartilage dividing your nose is shifted far enough to one side that it substantially restricts airflow on that side — gets dramatically worse at night because of the blood flow changes described earlier. If one side of your nose is always the worse one, if you’ve always been a mouth breather at night as far back as you can remember, or if your congestion is so severe that no amount of environmental optimization makes a real difference, a structural cause is worth ruling out with an ENT. Septoplasty addresses a deviated septum surgically and for many people is the turning point that makes nighttime breathing normal for the first time in their adult lives.
Nasal polyps are another structural cause of severe nighttime congestion that doesn’t respond well to conservative management — these are soft growths in the nasal passages that form after chronic inflammation and can block airflow significantly even when everything else is being managed well.
Sleep apnea is worth mentioning too. Chronic nasal congestion is a significant contributor to sleep apnea — when you can’t breathe through your nose, the airway mechanics during sleep change in ways that increase apnea risk. If you’re doing everything right for your sinuses and still waking up exhausted, unrefreshed, or with a headache, a sleep study is worth discussing with your doctor.
A Practical Nighttime Sinus Routine That Actually Works
Pulling it all together into something you can actually implement:
One to two hours before bed: Do your nasal rinse with an electric irrigator if you use one. This clears the day’s allergen and irritant accumulation before you seal yourself into your bedroom. Take a hot shower if possible — the steam opens passages and the timing means you go to bed at your clearest point of the evening.
Right before bed: A few sprays of plain saline in each nostril to keep the nasal lining moist. Nasal strips applied if you know you’ll struggle with airflow overnight. If you’re using a nasal steroid spray as prescribed, this is the time to use it — evening application tends to be more effective for nighttime symptoms.
In your bedroom: Humidifier running — not optional if the air is dry. Air purifier running on low or its auto setting. Allergen-barrier covers on your mattress and pillows. Head elevated with an extra pillow or wedge. These environmental conditions work passively through the whole night without you doing anything else.
What to avoid: Alcohol within a few hours of bed — it’s a vasodilator that causes nasal swelling. Decongestant spray as a nightly habit. Sleeping with pets in the room if dander is a trigger for you. Windows open during high-pollen seasons.
None of this is complicated. The reason most people with chronic nighttime sinus congestion are still suffering is that they’re addressing one piece in isolation — taking a decongestant, or running a humidifier, or buying a new pillow — rather than building the full environment that addresses all the reasons nighttime makes sinuses worse simultaneously. Stack these changes together and the cumulative effect is real and lasting.
Frequently Asked Questions
Why is only one nostril blocked at night?
This is the nasal cycle — your body alternates airflow dominance between nostrils roughly every 2 to 4 hours as a normal physiological process. When you’re horizontal, the lower nostril gets more blood pooling in its lining and tends to close off more completely. If you switch sides, that nostril clears and the other one closes. This is normal, but if one side is always dramatically worse than the other regardless of position, a structural issue like a deviated septum on that side is worth investigating.
Why do I wake up at 3 or 4 AM with sinus pressure?
This is partly the circadian rhythm of your immune response — inflammatory chemicals naturally peak in the early morning hours — and partly the cumulative effect of hours of horizontal positioning on nasal drainage. By 3 or 4 AM, you’ve been flat long enough for significant mucus pooling and tissue swelling to have built up. Head elevation and a good humidifier both help reduce how severe that 3 AM wake-up is.
Is it bad to sleep with a humidifier on all night?
No — running a humidifier overnight is generally beneficial for sinus health, with one important caveat. You want to keep humidity in the 40 to 50 percent range. Above that, you start creating conditions that dust mites and mold prefer, which can make allergen levels in the room worse. A humidifier with auto humidity sensing handles this automatically and is worth the upgrade for anyone using one regularly.
Can the position I sleep in make sinus congestion worse?
Yes, significantly. Sleeping on your back increases congestion because both sides experience the horizontal blood pooling simultaneously. Sleeping on your side concentrates the swelling in the lower nostril. Sleeping with your head elevated — regardless of position — is the most reliably helpful adjustment. Some people find sleeping on the side opposite to their worst nostril gives that nostril a chance to drain while the better side handles airflow.
Does eating before bed make sinus congestion worse?
It can, particularly for people with acid reflux. Stomach acid that reaches the back of the throat irritates the same passages involved in sinus drainage and can worsen post-nasal drip and nighttime congestion significantly. If your nighttime symptoms consistently include throat irritation and post-nasal drip, and you tend to eat within an hour or two of going to bed, that connection is worth paying attention to.
Final Thoughts From Me
Nighttime sinus congestion doesn’t have to be just something you endure. It has specific causes — gravity, dry air, allergens in your sleep environment, blood flow shifts, post-nasal drip — and each of those causes has a practical response. The people who still suffer every night are usually the ones who’ve tried one thing, found it helped a little but not enough, and stopped there.
The full picture works together. Elevation and humidity and clean air and allergen-barrier bedding and an evening rinse routine aren’t redundant — they’re each addressing a different piece of why nights are harder on your sinuses than days. Build the full environment, give it a couple of weeks to compound, and the difference in how you sleep and how you feel in the morning is the kind of change that makes you wonder why you waited so long to take it seriously.
If you’re still in the middle of figuring out what’s actually driving your sinus problems — whether it’s chronic sinusitis, allergies, a structural issue, or some combination — the full breakdown of why chronic sinusitis keeps coming back is a good place to start making sense of the bigger picture.
As an Amazon Associate we earn from qualifying purchases through some links in our articles.