Most people misidentify their headache type — and treat it wrong. Here’s how to tell a true sinus headache from a migraine, and what actually works for each.

Here is something that should genuinely frustrate you: studies have found that up to 90 percent of self-diagnosed “sinus headaches” are actually migraines.
Ninety percent. That’s not a rounding error — that’s almost everyone who thinks they have a sinus headache actually having something else entirely. And because the treatment for a sinus headache and the treatment for a migraine are completely different, most of those people are either not treating their headache at all, treating it with the wrong thing, or wondering why nothing seems to work.
I spent six years in an ENT and allergy clinic watching this play out over and over. Patients would come in convinced they had a sinus infection driving their headaches. The CT scan would be clear. The doctor would ask a few specific questions, and within five minutes it would become obvious the patient had been having migraines — sometimes for years — and had never been told. The relief in their face when someone finally explained what was actually happening was something I saw dozens of times. It’s one of the main reasons I started writing about this stuff.
So let’s sort it out properly.
Why Sinus Headaches and Migraines Get Confused So Often
The confusion is completely understandable once you know the anatomy. Your sinuses — the air-filled cavities in your skull behind your forehead, cheeks, and the bridge of your nose — sit right next to the same nerve pathways involved in migraine pain. When either condition flares, the pain lands in almost exactly the same location: pressure behind the eyes, across the forehead, in the cheekbones, sometimes at the top of the head.
Migraines also frequently cause nasal symptoms. Congestion, a runny nose, and a feeling of facial pressure during a migraine attack are common enough that they’re well documented in the research — they’re caused by activation of the trigeminal nerve system, which governs sensation across the whole face including the sinuses. So someone who gets a migraine with nasal congestion and facial pressure reasonably concludes they have a sinus headache, because that’s exactly what it feels like.
The pharmaceutical industry hasn’t helped. “Sinus headache” products like Sudafed and similar decongestants have been marketed aggressively for decades, which has baked the idea of the sinus headache as a common, distinct condition into the public consciousness. In reality, a true sinus headache — pain caused specifically by sinus inflammation from infection or blockage — is relatively uncommon compared to migraine, and it almost always comes with clear signs of acute sinus infection that go beyond just the headache.
What a True Sinus Headache Actually Is
A genuine sinus headache is caused by pressure and inflammation inside the sinus cavities themselves — typically during an acute sinus infection. The sinus lining swells, the openings that allow drainage get blocked, mucus backs up, and the resulting pressure creates pain that’s felt across the face and forehead.
The key word is infection. A true sinus headache doesn’t usually show up on its own. It comes as part of a package that includes thick discolored nasal discharge, fever or a feeling of being genuinely unwell, congestion that started as a cold or upper respiratory infection, and pain that’s noticeably worse when you lean forward or bend your head down — because that position increases the pressure inside the already-congested sinus cavities.
If you’re getting frequent headaches with facial pressure but no fever, no discolored mucus, and no clear infectious illness preceding them — and especially if those headaches last more than a day — the odds that they’re caused by active sinus infection are low. Something else is driving the pain, and migraine is by far the most common culprit.
That said, chronic sinusitis — where the sinuses are in a state of persistent low-grade inflammation rather than active infection — can contribute to a baseline of facial pressure and discomfort that’s genuinely sinus-driven. This is different from the acute sinus headache described above, and it’s part of why chronic sinusitis is so much more complicated to diagnose and treat than a simple sinus infection.
What a Migraine Actually Is — and Why It Feels Sinus-Like
Migraine is a neurological condition, not a vascular one and not a sinus one, despite what older explanations suggested. It involves abnormal activation of pain pathways in the brain — specifically the trigeminal nerve system — that creates pain, sensory sensitivity, and a cascade of other symptoms that vary significantly from person to person.
The trigeminal nerve is the reason migraines so often feel like sinus headaches. This nerve has three branches that cover sensation across the entire face — the forehead and eyes, the cheeks and upper jaw, and the lower jaw. When a migraine activates the trigeminal system, pain can be felt across any or all of those areas, which maps almost perfectly onto where sinus pain is felt. The trigeminal nerve also innervates nasal blood vessels, which is why nasal congestion and runny nose are genuine migraine symptoms rather than coincidental — the nerve activation directly affects nasal blood flow and secretion.
Migraines also frequently cause something called allodynia — where normally non-painful sensations become painful during an attack. Wearing glasses feels uncomfortable. Touching the face hurts. The scalp is tender. This contributes to the facial pressure sensation that makes patients think their sinuses are the problem when the pain is actually entirely neurological in origin.
The Diagnostic Checklist: Sinus Headache or Migraine?
Here are the questions that clinicians use to distinguish between the two. Go through them honestly — the pattern of your answers is more useful than any single response.
Signs That Point Toward a True Sinus Headache
- The headache started during or immediately after a cold or upper respiratory infection
- You have thick, yellow or green nasal discharge alongside the headache
- You have a fever or feel genuinely unwell and run-down, not just in pain
- The pain gets dramatically worse when you lean forward or tip your head down
- The headache is in a fixed location that corresponds to a specific sinus — forehead for frontal sinuses, cheekbones for maxillary sinuses
- The headache came on gradually over days alongside worsening congestion
- Decongestants genuinely relieve the pain, not just the congestion
- You don’t have nausea, light sensitivity, or sound sensitivity with the headache
Signs That Point Toward Migraine
- The headache occurs repeatedly, several times a month, often with similar patterns
- The pain is moderate to severe and genuinely disabling — not just uncomfortable
- You have sensitivity to light, sound, or smell during the headache
- Nausea or vomiting occurs with the headache
- The headache lasts 4 to 72 hours if untreated
- Physical activity makes the pain worse
- You had what felt like a warning period before the headache — mood changes, neck stiffness, increased thirst, fatigue — hours before the pain started
- Some attacks include visual disturbances — flickering lights, blind spots, zigzag patterns — before the pain begins (this is migraine aura)
- The headache responds to migraine-specific medication better than to decongestants
- There is no fever and no discolored mucus
If the majority of your answers fall in the migraine column — especially if you’re getting these headaches repeatedly without an identifiable infectious cause each time — migraine is the much more likely diagnosis and worth discussing with a doctor who takes it seriously.
The Overlap Zone: When It’s Both
One thing I saw frequently in the clinic that’s worth naming explicitly: some people genuinely have both conditions, and each one can trigger the other. Sinus inflammation and congestion can act as a migraine trigger in people who are susceptible to migraine — the pressure, the disrupted sleep, the mouth breathing that comes with congestion are all established migraine triggers. And a migraine that causes significant nasal symptoms can secondarily cause enough disruption to sinus drainage that it tips someone with underlying sinus inflammation into a true sinus flare.
This overlap is one of the reasons the two conditions are so chronically confused, and it’s why managing the sinus side of things — reducing inflammation, keeping your home environment clean, doing regular nasal irrigation — can sometimes reduce migraine frequency even in people whose primary diagnosis is migraine rather than sinusitis. The two systems are not independent.
If you’re dealing with chronic facial pressure that never fully resolves, the situation where your CT scan comes back normal but you still feel pressure every day is worth understanding — because that specific scenario is often where the migraine-sinus overlap is most pronounced and most mismanaged.
What Actually Works for Each
Treating a True Sinus Headache
If you have a genuine sinus headache from active sinusitis, the goal is to reduce the underlying inflammation and restore drainage so the pressure has somewhere to go.
Nasal decongestants — either oral like Sudafed or topical sprays — reduce the swelling in the nasal passages and sinus openings that’s causing the blockage. The Sudafed PE review here gives an honest breakdown of what to expect. The important caveat: topical decongestant sprays should not be used for more than three days consecutively or rebound congestion — worse than the original — sets in.
Saline irrigation physically flushes out the congested mucus and reduces inflammatory load in the sinuses. Done properly with an electric irrigator, it’s one of the most effective non-pharmaceutical interventions for acute sinus pressure. I’ve used the electric sinus rinse machines reviewed here during acute flares and the pressure relief afterward is immediate and real.
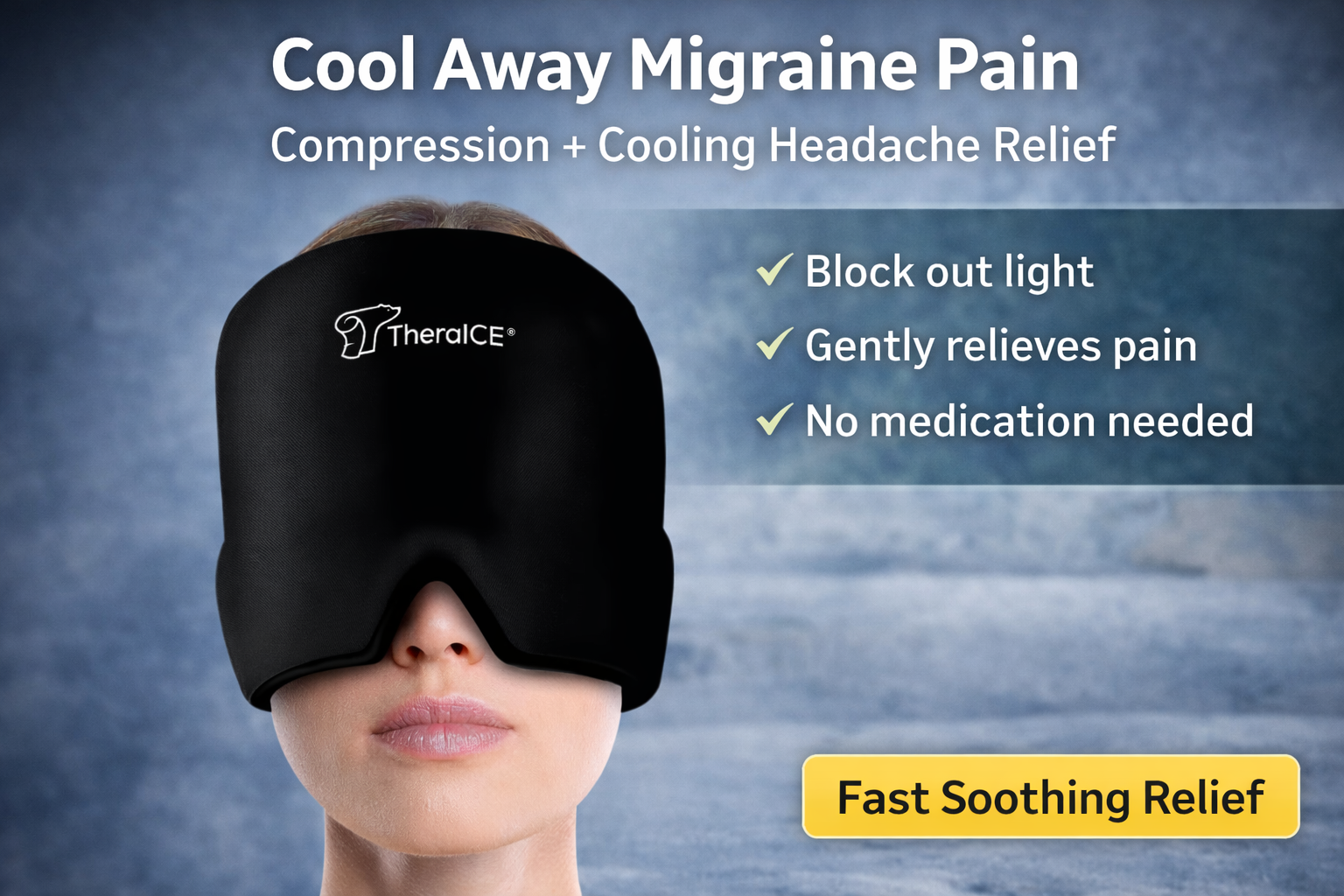
Cold therapy on the face reduces inflammation and numbs the pain signals coming from the sinus tissue. The TheraICE head wrap covers the full forehead, eye area, and temples simultaneously — which matters because sinus pressure rarely stays neatly in one spot — and the hands-free design means you can actually rest while using it rather than holding an ice pack in place.
Steam inhalation loosens thick mucus and temporarily opens sinus passages, providing real if temporary relief. A hot shower before bed during a sinus infection is the free version; a portable steam inhaler gives you a more concentrated version you can use any time.
Antibiotics are only appropriate if there’s a genuine bacterial infection — fever, prolonged symptoms beyond 10 days, symptoms that improved and then got significantly worse. Most acute sinusitis is viral and resolves without antibiotics. Pushing for an antibiotic prescription for every sinus headache is one of the most common and consequential mistakes people make.
Treating a Migraine
Migraine treatment is a whole subject of its own, but the fundamentals are important to understand if you’ve been misidentifying your headaches and using the wrong interventions.
Over-the-counter pain relief can work for mild to moderate migraines, particularly when taken at the very first sign of an attack before the pain fully develops. Excedrin Migraine — which combines acetaminophen, aspirin, and caffeine — is specifically formulated for migraine rather than general headache, and the caffeine component genuinely helps by constricting blood vessels and enhancing the absorption of the pain relievers. The full breakdown of Excedrin Migraine for sinus-adjacent head pain is worth reading if you’ve been relying on decongestants for headaches that haven’t been responding well.
Cold therapy works for migraine too, which is part of why the sinus-migraine confusion persists — the TheraICE cap that helps with sinus pressure is genuinely also used by migraine sufferers, because cold applied to the forehead and temples reduces the perception of migraine pain through the same nerve pathway mechanisms. It doesn’t treat the underlying neurological event, but it genuinely helps with the pain experience.
Triptans — prescription medications like sumatriptan — are migraine-specific drugs that work on the neurological mechanism of migraine directly. They don’t work on sinus headaches. If someone has been using triptans and getting relief, that’s actually strong evidence that they were having migraines rather than sinus headaches, because triptans don’t do anything for sinus pressure.
Identifying and managing triggers is the long-term management strategy for migraine that has no equivalent in sinus headache treatment. Common migraine triggers include disrupted sleep, dehydration, certain foods and drinks, hormonal fluctuations, strong smells, bright lights, and — relevant to this site — sinus congestion and inflammation itself. Keeping a headache diary for a few weeks to identify personal triggers is one of the most useful things a migraine sufferer can do, and it’s the foundation of any serious preventive approach.
When to See a Doctor — And What to Ask For
If you’ve been self-treating recurrent headaches as sinus headaches without much success, a doctor’s appointment is warranted — but going in prepared makes a significant difference in the quality of care you get.
Bring a brief headache diary if you can — even just two weeks of notes on when headaches occur, how long they last, what they feel like, and what accompanies them. This information transforms a vague complaint about recurring headaches into a pattern a clinician can actually work with.
Ask specifically about migraine. Many primary care physicians underdiagnose migraine because patients present with facial pain and nasal symptoms and the word “sinus” comes up first. If you’ve been through this loop, saying explicitly “I want to understand whether these might be migraines rather than sinus headaches” opens a different conversation than just describing the pain location.
An ENT is the right specialist if you have ongoing sinus symptoms alongside the headaches — chronic congestion, recurring infections, post-nasal drip, reduced smell — because ruling out a structural or chronic inflammatory cause is important before attributing everything to migraine. A neurologist is the right specialist if the sinus workup is clear and the headache pattern strongly suggests migraine. Sometimes you need both.
If headaches are a regular part of life and are significantly affecting your quality of life or sleep, that alone justifies getting proper answers. Nobody should be managing severe recurring headaches with decongestants indefinitely because they never got an accurate diagnosis.
The Sinus Connection to Headaches That People Miss
Even if your recurring headaches turn out to be migraines rather than sinus headaches, the state of your sinuses isn’t irrelevant. Chronic nasal congestion disrupts sleep — and poor sleep is one of the most reliable migraine triggers. The specific reasons sinus congestion gets worse at night and what to do about it are worth understanding even for migraine sufferers, because improving sleep quality by improving nighttime nasal airflow can meaningfully reduce migraine frequency.
Similarly, the indoor environment — the allergens and irritants in your home air — can drive both chronic sinus inflammation and the cascade of physiological stress that triggers migraine. Understanding what’s actually in your indoor air and addressing the highest-impact triggers reduces the overall inflammatory burden that feeds into both conditions.
The two conditions interact. Managing one tends to help the other, which is why a comprehensive approach to sinus health benefits people regardless of whether their primary diagnosis is sinusitis, migraine, or both.
Frequently Asked Questions
Can I have a sinus headache without congestion?
A true sinus headache — caused by acute sinus infection or significant sinus blockage — almost always comes with congestion and other signs of sinus disease. Facial pain without congestion, discharge, or infection is much more likely to be migraine or another type of headache disorder than true sinusitis. This is one of the clearest distinguishing features between the two conditions.
Why do my headaches get worse in spring and fall?
This seasonal pattern is common in both sinus headache and migraine, but for different reasons. High pollen counts in spring and fall drive allergic nasal inflammation in people with allergies, which can cause genuine sinus pressure headaches. But seasonal weather changes — shifts in barometric pressure, temperature swings, changes in light — are also established migraine triggers. Many people find their headache frequency increases in transitional seasons regardless of whether allergies are involved.
Is it possible to have a migraine that only affects one sinus area?
Yes. Migraine pain is frequently localized and can be felt specifically in the cheekbone, behind one eye, or across one side of the forehead — exactly where sinus pain is felt. Unilateral facial pain is actually more characteristic of migraine than of sinusitis, which tends to be bilateral and distributed across multiple sinus locations.
Should I try migraine medication even if I think I have sinus headaches?
This is worth discussing with your doctor. The classic clinical approach is sometimes to try a migraine-specific treatment — like a triptan — and see if it works. If it resolves the headache, that’s strong evidence for migraine. If it does nothing, other causes get investigated. This kind of diagnostic trial approach is common and reasonable, especially when the headache pattern fits migraine better than sinusitis.
Can weather changes cause sinus headaches?
Weather changes — specifically drops in barometric pressure before rain or storms — are a well-documented migraine trigger. They’re often blamed for “sinus headaches” because they’re atmospheric changes people associate with sinus discomfort. The underlying mechanism, though, is neurological rather than sinus-related for most people. True sinusitis-driven headaches don’t reliably follow barometric patterns the way migraine does.
Final Thoughts From Marcus
Spending years treating migraines with decongestants and sinus rinses — and getting partial, confusing relief — is an incredibly common experience and an incredibly avoidable one. The reason it happens isn’t that people are careless; it’s that the two conditions mimic each other well enough to fool even clinicians who aren’t specifically looking for the distinction.
What I saw repeatedly in six years of working alongside ENT physicians was that the diagnosis question — sinus or migraine? — was almost always answerable with a careful patient history. The symptoms, when laid out clearly, point in a direction. The pattern of what helps and what doesn’t points in a direction. And once someone was pointed at the right diagnosis and the right treatment, years of frustrating, ineffective management suddenly started making sense.
If this article has made you think your headaches might not be what you’ve assumed them to be, that’s worth following up on. A conversation with your doctor, a proper headache diary, and a willingness to consider migraine as the diagnosis is all it takes to get onto the right track. The treatment exists. The relief is real. You just need to be treating the right thing.
Written by Marcus T. — Marcus spent six years working as a patient advocate coordinator at an ENT and allergy clinic before leaving to manage his own chronic sinusitis full-time. During that time he sat in on hundreds of consultations, watched patients repeatedly misidentify their headache type, and saw firsthand how much time and money people wasted treating the wrong thing. He’s been writing about sinus health from that clinical-adjacent perspective ever since, combining what he absorbed in the clinic with his own daily experience managing sinus disease without surgery.
— Marcus T., Sinus Struggles
As an Amazon Associate we earn from qualifying purchases through some links in our articles.