Going through septoplasty recovery and not sure what to expect? Here’s the honest, week-by-week breakdown from someone who lived it — including the surprises nobody warns you about.

If you’re about to have septoplasty — or you’re sitting in your recliner right now wondering why nobody told you it would feel like this — this guide is for you.
I had septoplasty and sinuplasty done at the same time, and I want to be straight with you: recovery is harder than most people expect. Not impossible. Not dangerous. But harder. The online advice I found before my surgery was either too vague or suspiciously cheerful. “Most people return to work in a week!” Okay, sure. Most people also apparently don’t feel like they got hit by a truck for five days straight.
This guide covers everything — week by week, symptom by symptom — based on real experience and everything I’ve learned since. Whether you’re pre-op and researching, mid-recovery and panicking, or weeks out and still not feeling right, you’re in the right place.
What Is Septoplasty and Why Does Recovery Take So Long?
Before we get into the timeline, it helps to understand what actually happened to your body during that surgery.
Septoplasty is a procedure to straighten the nasal septum — the cartilage and bone that divides your nose into two sides. When it’s crooked or deviated, it blocks airflow on one or both sides. The surgeon goes inside your nose (no external cuts in most cases), trims and repositions the cartilage or bone, and stitches everything back up.
If you also had sinuplasty — where small balloon catheters are used to open up blocked sinus passages — your recovery is going to be more intense because more tissue and bone was disrupted.
The reason recovery takes weeks, not days, is swelling. The inside of your nose and sinuses has been physically manipulated, cut, and stitched. That swelling doesn’t peak immediately — it often gets worse before it gets better. Then there’s the healing of nerves, cartilage, and mucous membranes, all of which take much longer than regular skin.
This is also why the symptoms feel so all over the place. One day you’ll think you’re turning a corner, and the next you’ll be back on the couch wondering if something went wrong. That’s not a sign of failure — it’s just how this heals.
Before Surgery: What You Should Actually Prepare
Most surgeons give you a pre-op packet and a list of medications to stop taking. That’s important. But there are a few things I wish someone had told me that didn’t make it into any official packet.
Set Up Your Sleeping Situation Before Surgery Day
You will need to sleep with your head elevated — usually at a 30 to 45 degree angle — for at least the first week. Have your recliner ready, or stack your pillows in a wedge setup before you go in. Trying to figure that out when you’re groggy and in pain post-surgery is no fun.
Trim Your Nose Hair Before You Go In
This might sound oddly specific, but it’s genuinely important. Long nose hair near the surgical site causes friction and irritation when you’re already raw and swollen. Do it a few days before surgery, not right before. I wrote a full breakdown on exactly why it matters:
👉 Do I Need to Trim My Nose Hair Before Septoplasty?
Get Your Supplies Lined Up Before You Leave for Surgery
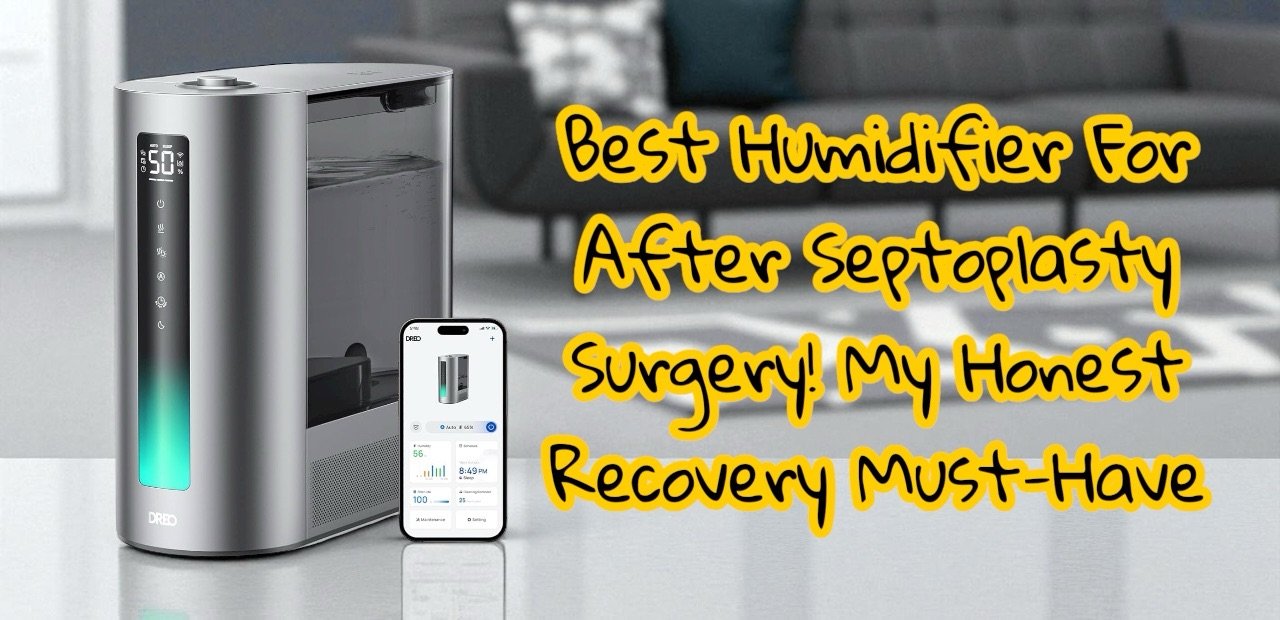
You’re going to need a few things the moment you get home. The most important are a good humidifier, an electric sinus rinse machine, and the right ice pack. Don’t wait until day two when you’re miserable to start shopping. Links to what actually worked for me are throughout this guide.
Plan for Two Weeks Off, Not One
If your boss or family is expecting you back in seven days, adjust those expectations now. You might feel okay-ish by day eight. But you might not. Having the second week carved out removes a layer of stress that genuinely makes recovery harder.
Days 1–2: Surgery Day and the Morning After
What to Expect Immediately After Surgery
You wake up from anesthesia and the first thing you notice is that your nose feels completely stuffed — like the worst congestion you’ve ever had, times ten. You might also have a gauze drip pad taped under your nostrils catching drainage from the surgery. That’s completely normal.
The pain on day one is manageable for most people because the surgical anesthesia is still wearing off and your prescriptions are fresh. Don’t let day one fool you. Day one is usually the best day of the first week.
If you had stents placed — silicone splints inside your nostrils to hold the septum in position while it heals — you’ll feel them. They feel like firm pieces of plastic blocking your airway. That’s because they are. It is uncomfortable. It is also temporary.
The swelling in your face will start building through day one and into day two. Your nose, upper lip area, and sometimes your cheeks will feel thick and tight. You will not be able to breathe through your nose at all. Mouth breathing is your life now for the next several days.
The Upper Lip and Tooth Pain Nobody Warns You About
One of the most surprising symptoms in the early days is pain in your upper lip, gums, and front teeth. Nobody warned me about this. If you’re experiencing it, it’s nerve-related — the infraorbital nerve that runs from the cheek down into the gums gets irritated from all the surgical trauma. It’s completely normal, even though it’s deeply unpleasant.
👉 Why Does My Upper Lip Hurt After Septoplasty?
What Helps in Days 1–2
Keep ice packs on your cheeks and around the bridge of your nose — not directly on the nose itself. Using the right ice pack makes a real difference when you’re trying to get through those first two days without losing your mind.
👉 The Only Ice Pack That Worked on My Septoplasty Pain
Run a humidifier constantly. When you can’t breathe through your nose at all, you’re mouth-breathing 24 hours a day, and dry air will crack your lips, dry out your throat, and make every symptom feel worse.
👉 Best Humidifier After Septoplasty: My Honest Recovery Must-Have
Stay on top of your pain medication schedule. Don’t wait until the pain spikes to take your next dose. Keeping the medication consistent makes a genuine difference in how manageable those first two days feel.
Days 3–5: The Hardest Part of Recovery
Let me prepare you for this stretch, because nobody prepared me, and it nearly broke me.
Days 3 through 5 are, for most people, the worst of the entire recovery. The swelling reaches its peak somewhere in here. If you had stents, they’re still in, which means you still can’t breathe through your nose. The nerve pain in your face is at its most intense. Sleep is nearly impossible. Everything hurts more than it did on day two.
There’s also an emotional component to this window that doesn’t get talked about enough. When pain is intense, unrelenting, and you can’t see any obvious improvement day to day, it’s very hard to stay calm. I had moments in this stretch where I genuinely questioned whether something had gone wrong, whether I’d made a mistake having the surgery, and whether I was ever going to feel normal again.
You didn’t make a mistake. Something didn’t go wrong. This is just what days 3 through 5 feel like.
Sinus Pressure in This Window
The pressure you feel during this stretch — that feeling of your whole face being packed solid and something pressing on your eyes from the inside — is one of the most commonly reported symptoms after nasal surgery. There’s a specific reason it gets so intense, and understanding why actually helps you manage it better.
👉 Why Sinus Pressure After Nose Surgery Feels So Intense
The Post-Op Mistakes That Make This Window Worse
A lot of people accidentally make days 3 through 5 harder on themselves by doing things they shouldn’t — blowing their nose too early, skipping rinses because they hurt, or not staying hydrated enough. I made several of these mistakes myself and paid for it.
👉 Post Sinus Surgery Care Mistakes That Nearly Ruined My Recovery
How to Get Through Days 3–5
- Ice packs in rotation — 20 minutes on, 20 minutes off, all day long
- Humidifier running in whatever room you’re in, especially overnight
- Head elevated even when resting — never lying completely flat
- Small sips of water constantly — dehydration makes sinus inflammation significantly worse
- Soft foods only — nothing that requires real chewing or wide jaw movement
- Pain meds on a consistent schedule, not just when it gets unbearable
- Rest, and more rest — your body is doing serious internal work right now
Hydration Matters More Than You Think
Staying hydrated during sinus recovery isn’t just general health advice — it directly affects how your sinus tissue heals and how thick or thin the mucus and drainage stays. Thick, sticky drainage is much more uncomfortable and much harder to rinse out.
👉 How Hydration Affects Sinus Healing — and the #1 Product That Helps
Day 7: Stent Removal — The Moment You’ve Been Waiting For
For most people, stent removal happens around day 7 at a follow-up appointment with your surgeon. I’m not going to sugarcoat it: the removal is uncomfortable. It feels strange and a little intense. But it’s over in seconds, and what follows is one of the more dramatic moments of the whole recovery.
You can breathe. Not perfectly — you’re still swollen — but compared to the wall of blocked nothing you’ve been living with all week, even partial nasal airflow feels like a miracle. The swelling will still be significant after stent removal. Don’t expect to feel completely clear. But you will feel meaningfully better, and that improvement tends to build from here.
Starting Nasal Rinses Properly
If you haven’t started nasal rinses yet, your doctor will likely have you begin around the time of stent removal. This is where having the right equipment matters enormously.
Using a standard neti pot or a cheap squeeze bottle after septoplasty is, at best, uncomfortable and ineffective. At worst, it can force water into areas that are still healing and cause significant pain. An electric sinus rinse machine — one with adjustable, gentle pressure — is a completely different experience.
👉 Best Electric Sinus Rinse Machine That Actually Works and Doesn’t Hurt
👉 Why This Cordless Nasal Irrigation System Works Better Than a Neti Pot
How to Clean Your Nose After Septoplasty
There’s a right way and a wrong way to clean the inside of your nose post-surgery, and a lot of people get this wrong because nobody walks them through it clearly before they leave the hospital.
👉 Best Way to Clean Your Nose After Septoplasty Safely at Home
Week 2: Slow Progress, Strange Symptoms, and the Sinus Flu
Week two is when a lot of people hit a wall they weren’t expecting. You went through the worst of the pain, the stents are out, and you’re thinking things should be getting steadily better now. Sometimes they do. And sometimes, around day 8 to 12, you get hit with what feels like a brutal sinus infection or flu.
This isn’t unusual. As the swelling shifts and the debris inside the sinuses starts moving, it can trigger a wave of awful symptoms — congestion that feels as bad as the worst day of surgery, facial pressure, fatigue, and drainage that looks genuinely alarming. In most cases, this isn’t an infection. It’s just the healing process being deeply unpleasant.
That said, there are signs that something more serious is happening. If you’re running a fever, seeing bright yellow or green drainage that won’t let up, or experiencing increasing pain rather than fluctuating pain, call your surgeon.
The Stitches Question
Week two is also when people start noticing their internal stitches more — or wondering where they went. Septoplasty stitches are usually dissolvable, which means they break down on their own without needing removal. But the timeline for that varies more than you’d expect.
👉 How Long Do Stitches Stay In After Septoplasty and Sinus Surgery?
Ear Symptoms in Week 2
A lot of people start noticing strange ear symptoms during the second week — clicking, pressure, a feeling like the ears won’t pop, or muffled hearing. This catches people off guard because the surgery was on the nose, not the ears. But the sinuses and ears are closely connected, and changes in sinus drainage and pressure absolutely affect the Eustachian tubes.
👉 Why Your Ears Constantly Click But Never Feel Open
👉 Why You Feel Dizzy But Not Spinning: The Sinus and Ear Connection
Weeks 3–4: Real Improvement, But Not a Straight Line
By weeks three and four, most people are feeling meaningfully better. The severe pain is gone. You can sleep in a more normal position. Eating and talking don’t require concentration anymore. You might even have a few hours where you forget you had surgery.
But here’s the honest truth: recovery from septoplasty is not a straight upward line. It’s more like a staircase with occasional slides backward. You’ll have a great day followed by a rough day. You’ll feel clear in the morning and congested by evening. That’s normal. It doesn’t mean you’re not healing.
Swelling inside the nose can take 3 to 6 months to fully resolve. The full breathing results of septoplasty often aren’t felt until that swelling is completely gone. Some people don’t experience the full improvement until 6 months post-surgery. If you’re at week four and still not breathing as well as you hoped, don’t panic — the healing isn’t done yet.
Managing Your Home Environment During Recovery
One thing that makes a real difference during the longer recovery stretch is your indoor air quality. Dry air, dust, pet dander, and airborne particles all irritate healing sinus tissue and slow recovery down. This is when an air purifier in your bedroom becomes a practical recovery tool, not a luxury.
👉 A Powerful Air Cleaner That Targets Sinus Triggers Fast
👉 Air Quality Monitor — See What’s Triggering Your Sinus Problems
Month 2 and Beyond: What Full Recovery Actually Looks Like
By month two, the dramatic symptoms are behind you. What remains is a gradual, ongoing process of the internal tissue settling, cartilage firming up, and swelling continuing to decrease.
Some people notice that one side of their nose still feels more restricted than the other for months after surgery. This is common and usually resolves as swelling decreases. Some people also go through a phase around 6 to 8 weeks where things seem to get slightly worse before getting better again — this corresponds to a shift in how the scar tissue is forming inside.
Follow up with your surgeon at every scheduled appointment. These aren’t just checkboxes. Your doctor needs to see how the septum is healing, whether any scar tissue is forming in a way that needs to be addressed, and whether your sinuses are draining properly.
When Your CT Scan Is Normal But You Still Feel Pressure
This is one of the most frustrating things people experience after sinus surgery — and honestly, even without surgery. You go back to the doctor, they do a CT scan, it comes back normal, and yet you still feel pressure, congestion, or heaviness in your face every single day. This doesn’t mean nothing is wrong. There are real explanations for this that have nothing to do with the surgery failing.
👉 Why Your Sinus CT Scan Is Normal But You Still Feel Pressure
Symptoms That Look Alarming But Are Usually Normal
Part of what makes septoplasty recovery so stressful is encountering symptoms that seem alarming when they’re actually expected parts of healing. Here are the ones that catch people most off guard:
- Thick, discolored drainage in weeks 1–2 — usually old blood and mucus mixing together, not infection
- A smell that seems off or different — your olfactory nerves are adjusting to the changes inside your nose
- Feeling like you have a bad cold for weeks — the congestion is swelling, not illness, and it takes time to resolve
- Upper lip and tooth pain — nerve irritation from surgery, fully explained here
- Ear pressure, clicking, or muffled hearing — your Eustachian tubes responding to sinus pressure changes
- Feeling dizzy or off-balance — connected to the sinus and inner ear pressure relationship
- One side more clear than the other — completely normal as swelling resolves unevenly
- Feeling worse some days than others well into week three — not a setback, just how healing actually goes
When to Actually Call Your Surgeon
Most of what you experience during septoplasty recovery is uncomfortable but expected. However, there are legitimate warning signs that need medical attention. Don’t ignore these:
- Fever above 101°F (38.3°C) that doesn’t respond to Tylenol
- Bleeding that soaks through multiple gauze pads or won’t slow down
- Vision changes of any kind — blurred vision, double vision, or pain behind the eyes
- Severe headache that is dramatically worse than your normal post-op discomfort
- Swelling or redness spreading to your cheeks or around your eyes
- Pain that is sharply increasing after day 5 rather than gradually improving
- Signs of abscess — extreme tenderness in one localized spot, warmth, or hardness under the skin
When in doubt, call. Your surgeon’s office would always rather hear from you than have you sit at home with something that needed treatment.
The Recovery Supplies That Actually Made a Difference
I want to be honest about what helped and what was a waste of money. Here’s what I’d recommend to anyone going through this:
A Humidifier — Non-Negotiable
Running a humidifier through the first few weeks is one of the single most impactful things you can do for your comfort and your healing. Dry air slows mucosal healing, dries out your throat and mouth when you’re forced to breathe through them, and makes the congestion feel significantly worse. I used one in the bedroom every night for the first month.
👉 Best Humidifier After Septoplasty: My Honest Recovery Must-Have
👉 Smart Humidifier Review — The Best Way to Stop Dry Sinus Pain Fast
An Electric Sinus Rinse Machine
Once your surgeon clears you to start rinsing — and they will — do yourself a favor and skip the neti pot. Electric sinus rinse machines are gentler, more controlled, and far more effective at clearing the debris that builds up during healing. The difference is significant.
👉 Best Electric Sinus Rinse Machine for Congestion Relief: What Really Works?
👉 The Powerful Sinus Rinse System That Actually Clears You Out
The Right Ice Pack
Not all ice packs work well on a post-surgical face. You need something that conforms to your cheeks and the sides of your nose, stays cold long enough to matter, and doesn’t apply direct pressure to the nose itself. I went through a couple before finding one that actually helped.
👉 The Only Ice Pack That Worked on My Septoplasty Pain
A Good Nose Hair Trimmer for After Recovery
Once you’re healed, maintaining your nose hair properly becomes more important — especially if you’re prone to sinus issues. Trimming before surgery matters, and having the right tool for ongoing maintenance matters too.
👉 The Best Nose Hair Trimmer I Wish I Used Before My Sinus Surgery
Frequently Asked Questions About Septoplasty Recovery
How long does septoplasty recovery take?
The most intense symptoms — severe pain, total nasal blockage, stents — typically resolve within the first 1 to 2 weeks. Functional recovery, where you feel well enough to work and live normally, usually happens by weeks 3 to 4. Full healing, including the internal cartilage and the resolution of all swelling, takes 3 to 6 months.
When can I blow my nose after septoplasty?
Most surgeons say to avoid blowing your nose for at least 2 weeks, and some recommend waiting longer. Blowing creates pressure inside the nasal cavity that can disturb healing tissue, dislodge clots, or cause bleeding. Rinses are the way to clear your nose during recovery — not blowing.
Will I be able to breathe better after septoplasty?
For most people, yes — significantly better. But don’t expect to feel it immediately. The swelling from surgery temporarily makes breathing feel worse before it gets better. Full breathing improvement is often not felt until 3 to 6 months post-surgery when all the internal swelling has resolved.
Is it normal to still feel congested weeks after septoplasty?
Yes. Persistent congestion weeks after surgery almost always comes from swelling, not from the surgery failing. The inside of your nose needs months to fully settle. If you feel like you have a cold every single day even well after surgery, there’s a specific reason for that worth reading about.
👉 Why You Feel Like You Have a Cold Every Day (And It Won’t Go Away)
Can I exercise during septoplasty recovery?
Light walking is usually fine within a week or two, but anything that significantly raises your blood pressure or heart rate — running, lifting, intense cardio — should wait until your surgeon clears you. Elevated blood pressure increases the risk of post-op bleeding and can make swelling significantly worse.
What if I still feel pressure months after surgery?
This is more common than you’d think, and it can be genuinely maddening. Sometimes the CT scan comes back normal and yet the pressure and heaviness in your face is still very real. There are several explanations for this that have nothing to do with surgical failure.
👉 Why Your Sinus CT Scan Is Normal But You Still Feel Pressure
What I Know Now That I Wish I’d Known Before
If I could go back and tell myself one thing before surgery, it wouldn’t be about a specific product or technique. It would be this: give yourself permission to have a hard recovery without interpreting it as failure.
I went in expecting a week of being uncomfortable and came out of it needing almost three weeks before I felt like a functional human again. That gap between expectation and reality made an already difficult experience feel much worse than it needed to. Recovery is hard. It’s also finite. It ends.
The nose you’re recovering toward — one that actually lets air through properly, one that doesn’t block your sleep or make every head cold last three weeks — is worth the miserable stretch to get there. Most people who have septoplasty say, once they’re fully healed, that they’d do it again.
I’m one of them.
If you’re in the thick of it right now, hang in there. Read through the specific posts linked throughout this guide whenever you hit a symptom that scares you — because odds are, someone else went through exactly the same thing and wrote about it. You’re not alone in this.
👉 My Brutally Honest Septoplasty & Sinusplasty Recovery Timeline
As an Amazon Associate we earn from qualifying purchases through some links in our articles.